Sometimes all it takes to make transformative changes in healthcare delivery is seeing great ideas and being willing to “steal shamelessly.” Today, we share great ideas that have been developed and implemented around the world using the PFCC Methodology and Practice (www.pfcc.org). We hope you will steal them shamelessly “as is” and/or use them as a jumping off point to generate your own patient- and family-centered care initiatives.
Community Welcome
Alberta, Canada
At the Rockyview General Hospital in Alberta, Canada, a bi-weekly , three-hour session has been added to the staff orientation program to introduce all new employees to patient- and family-centered care. The session includes a tour of the site as seen through the eyes of patients and families to acquaint them with the kind of experience the hospital strives to provide its patients and families. At the conclusion, all session attendees are asked to fill out a commitment card that is placed on the entrance wall of the hospital.
, three-hour session has been added to the staff orientation program to introduce all new employees to patient- and family-centered care. The session includes a tour of the site as seen through the eyes of patients and families to acquaint them with the kind of experience the hospital strives to provide its patients and families. At the conclusion, all session attendees are asked to fill out a commitment card that is placed on the entrance wall of the hospital.
Pediatric Asthma: Improving Patient and Staff Experience
West Midlands, England
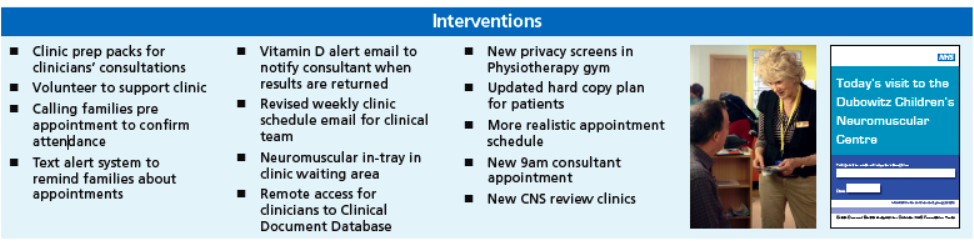
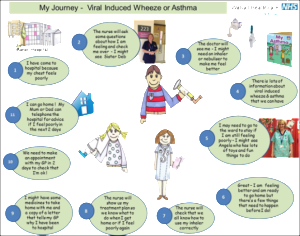
Overseen by a PFCC Guiding Council that meets weekly, multidisciplinary frontline care teams at Walsall Healthcare NHS Trust implemented several changes to improve the patient-centeredness of their care delivery. One simple, but powerful initiative they undertook was to design a patient journey map which is now provided to patients on arrival to give them a pictorial representation of what to expect through the department.
The Butterfly Project
Kelowna, British Columbia, Canada
 Kelowna General Hospital’s inpatient staff requested signage to alert all staff to enter patient rooms with greater sensitivity when a crisis is taking place in the life of a patient. Its maternity unit had already been using a Butterfly symbol to signify an infant death; the PFCC team expanded use of the image to include a severe crises (as determined by the care team), such as imminent death or death. This initiative has spread through the hospital and to other hospitals in the region; beforehand, there was no uniform way to alert staff when extra sensitivity is needed.
Kelowna General Hospital’s inpatient staff requested signage to alert all staff to enter patient rooms with greater sensitivity when a crisis is taking place in the life of a patient. Its maternity unit had already been using a Butterfly symbol to signify an infant death; the PFCC team expanded use of the image to include a severe crises (as determined by the care team), such as imminent death or death. This initiative has spread through the hospital and to other hospitals in the region; beforehand, there was no uniform way to alert staff when extra sensitivity is needed.
Outpatient Review Clinic for Boys with Duchenne Muscular Dystrophy
London, England
Great Ormond Street Hospital for Children NHS Foundation Trust was determined to improve the care experience for boys with Duchenne Muscular Dystrophy. Following the PFCC methodology, their team implemented a variety of patient- and family- centered interventions for the 3-4 hour multidisciplinary outpatient clinic visit. Results were impressive. The percentage of families receiving a care plan on arrival increased from 25% to 91%, wait times of under 30 minutes increased from 58% to 92%, and more than 90% of families report that their child’s concerns were listened to and their management plan was explained in a way that families understand.
Patient and Caregiver Empowerment
Staffordshire, England
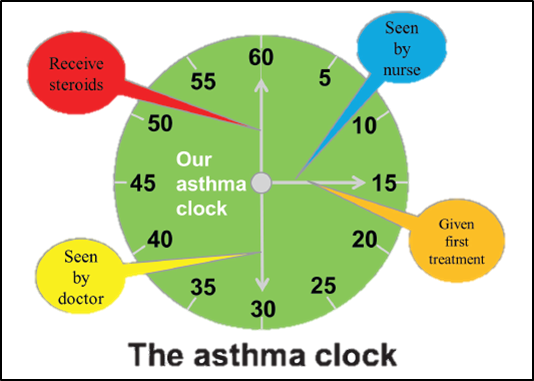
 As part of a children’s asthma improvement project, University Hospital of North Staffordshire sought to better understand the patient, family and staff experience of asthma care and to address barriers to excellent care. As a result of their PFCC efforts, all patients are now issued an asthma clock that reflects the ideal scenario for receiving care. Now the staff has a standard to guide them, and patients and their caregivers are encouraged to inquire with staff if there is a delay.
As part of a children’s asthma improvement project, University Hospital of North Staffordshire sought to better understand the patient, family and staff experience of asthma care and to address barriers to excellent care. As a result of their PFCC efforts, all patients are now issued an asthma clock that reflects the ideal scenario for receiving care. Now the staff has a standard to guide them, and patients and their caregivers are encouraged to inquire with staff if there is a delay.
Editor’s Note:
First developed in 2006 at the University of Pittsburgh Medical Center, the PFCC Methodology and Practice has been used successfully by more than 30 healthcare organizations around the world to engage patients as full partners in redesigning care delivery. For an overview of this simple, six step approach, you can read an earlier post the author wrote for EngagingPatients.org. Or, contact Patty Embree at Embreepl@upmc.edu .






1 Comment
thanks for sharing Pamela – hoping to add more case studies from the UK soon!