Enter the words “engaging patients” into Google’s search engine and you will see over 35 million results, surely an indication that patient engagement is very high on the radar screen for many of us in health care. And rightly so. Active participation in care delivery is an important element in not only patient satisfaction but is increasingly being shown to result in better outcomes and lower costs.
In our efforts to engage and partner with patients, the questions health care providers often struggle with are the “how?” and the “then what?” How do we get started? How do we go about engaging patients in defining ideal care delivery, how do we best influence their active participation in their plan of care, and what do we do with the information they provide us? It turns out that it isn’t as hard as you’d think.
The PFCC Methodology and Practice (PFCC M/P), developed at the University of Pittsburgh Medical Center in 2006, is a simple-to-learn and simple-to-implement six-step approach to engaging patients as full partners in redesigning care delivery. In use in over 60 different clinical conditions or care experiences at UPMC and increasingly being adopted outside of UPMC, the PFCC M/P is effective in any care setting – pre-hospital services, outpatient, inpatient, and post-hospital services. And in the best case scenario, the PFCC M/P is used to address communication and transitions in care between all of these segments of the full continuum of care.
While survey data, letters, and focus groups provide important information that we review and address, after-the-fact information can be hard to use effectively. It’s difficult to determine root causes after-the-fact and data alone can be dry.
One of the key elements of the PFCC M/P is Shadowing patients and families in real-time throughout each step of their health care journey. Shadowing enables us to view all care as experiences through their eyes, providing the emotional connection and that “aha” moment that creates urgency to drive change. We can use what we learn about the current state through Shadowing to form cross-functional teams that break down the silos and close the gaps between the current and ideal states of care delivery.
But Shadowing isn’t the only step in which we engage patients and families — we engage them at every one of the six steps of the PFCC M/P:
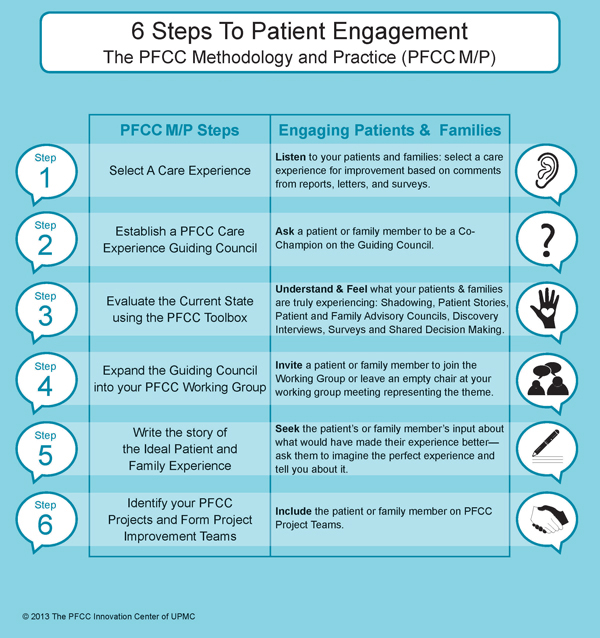
Click the image above to download the 6 Steps.
Engaging patients and families need not be a perplexing problem and the steps we take to improve care delivery based on their input need not come at a cost. Indeed, we have completed hundreds of PFCC projects based on what we’ve learned through Shadowing — projects that have added no cost and have resulted in decreased waste and cost. Changes are achieved by refocusing existing resources.
The next time you find yourself thinking about patient engagement and wondering where to begin, you might consider starting by Shadowing patients and families and sharing your observations across your care team. Understanding the opportunities to more effectively meet and exceed the needs and desires of patients and families is a powerful way to engage them in designing, and redesigning, care delivery.
Shadowing Guides (and all of the tools you’ll need if you decide to pursue the other steps of the PFCC M/P) are available to download at www.pfcc.org. You may also want to attend one of our free webinars (www.pfcc.org/webinars/) or register for our next workshop (www.PFCCVisionQuest.org/) which is scheduled for October 10-11 in Pittsburgh.
We welcome questions, comments, and suggestions and we would enjoy hearing your ideas for engaging patients and families (greenhousepk@upmc.edu)!





1 Trackback