As healthcare providers recognize the essential need to engage patients and to understand what is important to them in their health and healthcare delivery, there is need for a paradigm shift in the focus of “what’s the matter?” to “what matters to you?,” a concept put forward by Maureen Bisognano, President of the Institute for Healthcare Improvement. To explore what matters to patients undergoing total hip or knee replacement at The Bone and Joint Center of Magee-Womens Hospital of UPMC, we have implemented the “What Matters to You?” pilot project.
As healthcare providers recognize the essential need to engage patients and to understand what is important to them in their health and healthcare delivery, there is need for a paradigm shift in the focus of “what’s the matter?” to “what matters to you?,” a concept put forward by Maureen Bisognano, President of the Institute for Healthcare Improvement. To explore what matters to patients undergoing total hip or knee replacement at The Bone and Joint Center of Magee-Womens Hospital of UPMC, we have implemented the “What Matters to You?” pilot project.
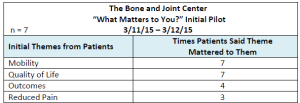
In our initial pilot, we posed this question to seven patients before surgery and again at their one-month post-operative visit. First we asked (at the pre-surgical office visit),”Thinking ahead in the process of your joint replacement surgery, what matters to you?” This is an open-ended question and patients were able to answer with as many responses as they wished. The results from these patients pertained to longer-term outcomes and were easily grouped into the following themes:
To further understand what matters to patients during each phase (pre-hospital, hospital and post-acute) of the care experience, we then expanded the pilot to 25 additional patients and revised our inquiry to two separate questions, “What matters to you before surgery, during your hospital stay and in the first three months following surgery?” and “What matters to you moving forward after you’ve recovered from your joint replacement?” In the expanded patient cohort, the themes from the initial pilot carried over but additional themes emerged, as well. The second set of responses is grouped into six overarching themes: outcomes, reduction in pain, quality of care/staff, education, quality of life, and environment of care.
Responses for these themes include:
1. Outcomes – infection, prosthesis success, dislocation, recovery time, surgical risks, pre-existing condition, weight control, nutrition, anesthesia
2. Reduction in pain
3. Quality of care/Staff – trust in MD, responsiveness and attitude of staff, meals, physical therapy 4. Education – overall education, exercise
5. Quality of life – mobility, resume activities of daily living, return to work
6. Environment of care – cleanliness, noiselessness, private room, sleep interruption
Moving forward, at the time of the four week follow-up visit, the patient’s previous responses to the question, “What matters to you before surgery, during your hospital stay and in the first three months following surgery?” will be reviewed with them. Now that they’ve been through the process, they’ll also be asked if their expectations were met and, retrospectively, if they would identify any new concerns when initially interviewed. We’ll also review previous responses to the question, “What matters to you moving forward after you’ve recovered from your joint replacement?” and patients will be asked if they would they feel the same way now that they are on their way to recovery.
As Bisognano so clearly illustrated in her keynote talk at the 25th IHI National Forum about engaging patients to understand their health goals, what health means to a 96-year-old (living pain-free) or a young mother-to-be (peer support through group pre-natal sessions) or an athlete with diabetes (the double-bang-for-the-buck of eating healthily) is the most important thing for us to understand. As the pilot project in The Bone and Joint Center shows, it doesn’t need to take a great deal of time and resources to make this paradigm shift; rather, it simply takes an acknowledgement that “What Matters to You?” is the essential question.
Editor’s note:This contribution was first published by the Patient and Family Centered Innovation Center’s online newsletter in May, 2015. Further insights about patient-centered care can be found in their newly launched blog at http://blog.pfcc.org/