Frances Hesselbein, a giant in the field of leadership development, says, “Culture does not change because we desire to change it. Culture changes when the organization is transformed; the culture reflects the realities of people working together every day.” The simplicity of this statement only underscores its importance. The problem, of course, is how do we get staff working together every day in a way that changes the culture of healthcare organizations, particularly in pursuit of patient-centered care?
The six-step Patient and Family Centered Care Methodology and Practice (PFCC M/P) affords that opportunity. It provides a path that has consistently proven its transformative powers in hundreds of healthcare settings over the past decade.
Drawn Together in a Common Mission
The magic begins in the way that the PFCC M/P brings together staff from all functions and levels of an organization into PFCC Working Groups. These teams include doctors, nurses, therapists and technicians, as well as parking attendants, schedulers, billers and housekeepers. They are representatives from all areas of the healthcare setting that have impact on the experience of patients and families. They meet weekly to identify and close the gaps between the current and ideal states of care delivery – from the viewpoint of patients and families who are full partners in co-designing the ideal care experience.
Gaining an ‘Enlightened Understanding’ 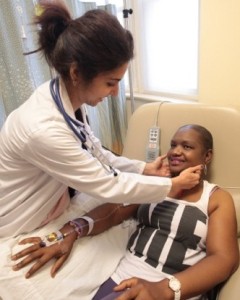
Empowered with tools such as Shadowing — direct, real-time observation and engagement with patients and families– PFCC Working Groups are able to identify every step of patients’ and families’ healthcare journeys to get a true picture of the current state of care. Tim Brown, founder and CEO of the experience-based design firm, IDEO, explains that direct observation — as opposed to after-the-fact comments and data — leads to an enlightened understanding of the experience, which leads to insights and those “ah-ha” moments. It creates an urgency to drive change and that, in itself, is a powerful motivator for those who impact patient and family experiences in the healthcare setting.
A Very Fine Collaboration
Collaborating regularly and continually in this way benefits both the organization and individual team members. Team members feel a sense of purpose and greater joy in the workplace because they have the tools to provide superb care experiences. They become greater than the “sum of their parts,” developing into high-performance care teams of people who are bound together by a common mission.
The structure of PFCC Working Groups also serves the very important function of breaking down silos, which are ubiquitous in healthcare. Silos exist between roles –nurses, doctors, administrators, transport staff, food services, etc. Between care settings — emergency room, operating rooms, inpatient units, etc. Between medical/surgical units — (cardiology, orthopaedics, mental health, trauma services, etc. And all along the care continuum between pre-hospital services, inpatient care, outpatient clinics, rehabilitation and long-term care, etc. Each of the individual “units” has its own culture within the larger organizational culture, the latter more diffuse and less able to permeate and penetrate down to the unit and individual level.
Building a New Culture
When the traditional silos are broken down, and individuals from every function and level of the organization have the opportunity to collaborate led by a common mission, a new culture is created. And as more PFCC Working Groups are formed and more staff members are added to PFCC Working Groups and project teams, the cultural impact grows.
A Framework for a True Transformation
Indeed, culture does not change simply because we proclaim that it must or say that our organization is pursuing a new culture. It requires a framework, a structure, a way to break down silos, and a way to bring together those who are bound by a common mission. In healthcare, the common mission that drives us to choose this as a career is providing exceptional care delivery to patients and families.
The PFCC Methodology and Practice provides what’s needed for true culture change. For more insights about the PFCC Methodology and Practice visit www.PFCC.org, read their blog at www.myPFCC.org or contact Patty Embree at embreepl@upmc.edu.





1 Trackback