
I have a confession to make – I love technologies that substitute for oftentimes slow human interactions. At the grocery store and at Home Depot, I head straight to the self-service lane where I quickly scan and pay for my items at a check-out kiosk. Further, I revere my online banking portal with the same affection that I have for sliced bread. Lastly, the success of my holiday shopping is measured by the ratio of the value of gifts purchased via the web compared to those procured with the crowds in brick-and-mortar stores.
PX2016: Improving Patient Experience
It is thus with satisfaction that I noted that more than half of the sponsors of the 2016 Beryl Institute Patient Experience Conference (PX2016) were technology firms. All of us (Taylor Healthcare included) endeavor to advance patient experience via software tools and resources designed to more efficiently improve the care and well-being of the patients we serve. PX2016 is the largest, independent, non-provider-hosted event that brings together healthcare professionals from around the world to share insights on improving patient experience. I participated in PX2016 – held April 13-15 in Dallas – for the first time in what I hope will be many years attending this event.
Extending Care Beyond the Hospital
 A current area of interest for me is extending patient care outside the walls of the hospital. To that end, I attended a session entitled, “Success of Discharge Calls to a Transitional Call Center.” A team at White Plains Hospital described a call-back program for their outpatients and ED patients that have remarkably pushed satisfaction scores for those populations ahead of those reported by their inpatients. One of the points made by the presenters was the challenge that patients had recalling discharge instructions and the negative impact that not understanding discharge instructions had upon satisfaction scores.
A current area of interest for me is extending patient care outside the walls of the hospital. To that end, I attended a session entitled, “Success of Discharge Calls to a Transitional Call Center.” A team at White Plains Hospital described a call-back program for their outpatients and ED patients that have remarkably pushed satisfaction scores for those populations ahead of those reported by their inpatients. One of the points made by the presenters was the challenge that patients had recalling discharge instructions and the negative impact that not understanding discharge instructions had upon satisfaction scores.
The Road to Recovery
As I listened to the providers from White Plains, I remembered an anecdote once shared with me by Steve Pratt, MD, an assistant professor at Harvard Medical School and practicing anesthesiologist at Beth Israel Deaconess Medical Center. Dr. Pratt noted that after surgery he would visit his patients, remind them that they had undergone general anesthesia, and explain that for the next 24 hours they should not drive or operate machinery, nor should they make important decisions or sign legal documents. Dr. Pratt dryly commented that he would then move aside so the nursing team could step in to describe the detailed discharge instructions that the patient would need to follow in order to ensure a successful recovery.
Reducing Readmissions
The challenge of optimizing when we elect to engage patients with their aftercare plans is not unique to any one organization. Significantly, the presenters from White Plains explained that their call-back operators had a copy of the patient’s discharge instructions at their fingertips to ensure that they were well-positioned to reinforce those instructions with the patient and answer any questions. Here, I was reminded of an initiative at the Portland VA Medical Center that automated their discharge instructions resulting in a three-fold decrease in their 14-day readmission rate. The improvement observed in Portland was due in large part to the on-call nurse having instant access to the discharge instructions that could then be reinforced with the patient, precluding a return visit to the hospital.
The Role of Technology
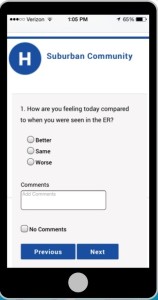 While technology by itself may not be the answer to improving patient experience, it can certainly play a role. In “Digital Engagement of Discharged ED Patients is a Must,” patient experience professionals from Edward-Elmhurst Health described a system for checking on patients the day after discharge with a short survey delivered via text or email. The presenters noted that a text message is generally perceived as less intrusive than is a phone call. The roughly 1 out of 20 patients who report an issue with medications, follow-up appointments or discharge instruction, are, in turn, flagged by the system to receive a call from a member of the Edward-Elmhurst Health clinical team.
While technology by itself may not be the answer to improving patient experience, it can certainly play a role. In “Digital Engagement of Discharged ED Patients is a Must,” patient experience professionals from Edward-Elmhurst Health described a system for checking on patients the day after discharge with a short survey delivered via text or email. The presenters noted that a text message is generally perceived as less intrusive than is a phone call. The roughly 1 out of 20 patients who report an issue with medications, follow-up appointments or discharge instruction, are, in turn, flagged by the system to receive a call from a member of the Edward-Elmhurst Health clinical team.
This hybrid approach – employing technology to screen for those patients with issues – resonated with the PX2016 attendees. The system employed by Edward-Elmhurst – an organization with satisfaction scores in the 99th percentile – also had the ability to support traditional call-backs to those patients who did not possess a means to receive a text or email message, as well as those patients who did not respond within an appropriate window of time.
Augmented Care
Reflecting on the Beryl PX2016 Conference, I am reminded that technological innovations that are so attractive to me in my healthy state cannot be universally applied to an ill population. As hospitals endeavor to discharge us quickly to our homes – our preference in most cases – we are rarely functioning at 100 percent capacity. At those times, our myriad of apps and Fitbit-style devices may abandon us. We may, however, still be able to navigate a relatively simple text message or phone call. Those well-being checks are instrumental to ensuring that we are progressing as expected, have no outstanding questions and are enjoying an exceptional care experience.




