 Improving the patient-centeredness of healthcare is “the right thing to do.” That being said, it also happens to make great business sense. A spotlight has been placed on patient-centered care, patient experience, and patient engagement under the Affordable Care Act (ACA) of 2010. The law sets forth financial incentives and penalties for providers and organizations that do not meet certain benchmarks that are commonly used (whether the measurement tools are appropriate is another topic for another day!) to measure patient experience.
Improving the patient-centeredness of healthcare is “the right thing to do.” That being said, it also happens to make great business sense. A spotlight has been placed on patient-centered care, patient experience, and patient engagement under the Affordable Care Act (ACA) of 2010. The law sets forth financial incentives and penalties for providers and organizations that do not meet certain benchmarks that are commonly used (whether the measurement tools are appropriate is another topic for another day!) to measure patient experience.
Soft Touch, Hard Benefits
Often, the terms ‘patient-centered care’ and ‘patient experience’ conjure up thoughts about the soft stuff – amenities (food, parking, wait times, way-finding…) or the need for clinicians to spend more time face-to-face speaking with patients. Patient experience is about the amenities – but much, much more. It is also about patient safety. It’s about breaking down silos that prevent coordinated, effective and timely diagnosis and treatment. Moreover, it’s about improving efficiency, creating effective patient education and preventing unnecessary readmissions.
Accelerating Progress
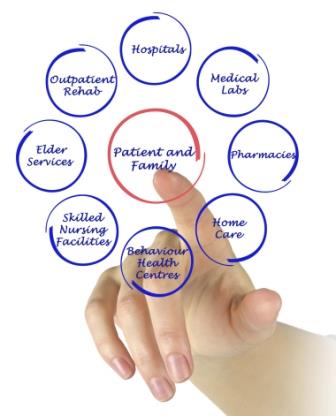
 Over the past 10-15 years, clinicians and healthcare organizations have been spending a great deal of time and effort, with the best of intentions, to improve safety, quality, experience, and costs. Yet, progress has been slow. However, more and more providers are finding that by employing the Patient and Family Centered Care Methodology and Practice (PFCC M/P), they can improve outcomes and experiences, and lowers costs. A six-step approach that is simple to learn and implement, the value of the PFCC M/P has been shown in over a dozen peer-reviewed scholarly publications. Importantly, it has proven to be replicable, sustainable (continuity is built into the six steps), and it makes good business sense.
Over the past 10-15 years, clinicians and healthcare organizations have been spending a great deal of time and effort, with the best of intentions, to improve safety, quality, experience, and costs. Yet, progress has been slow. However, more and more providers are finding that by employing the Patient and Family Centered Care Methodology and Practice (PFCC M/P), they can improve outcomes and experiences, and lowers costs. A six-step approach that is simple to learn and implement, the value of the PFCC M/P has been shown in over a dozen peer-reviewed scholarly publications. Importantly, it has proven to be replicable, sustainable (continuity is built into the six steps), and it makes good business sense.
The Power of the PFCC Methodology
By engaging with patients and families as full partners in redesigning care delivery, the PFCC M/P:
- Is a no-cost approach to transforming healthcare
- Identifies opportunities, and provides the mechanism, to improve the experience of care as defined by patients and families at each step of the health care journey
- Identifies and addresses patient experience quickly, without the limitations of after-the-fact, time-delayed assessments
- Creates a sense of urgency among the care team to drive and sustain change
- Creates high performance care teams of staff members at every level of the organization
- Breaks down silos functionally, hierarchically, and between segments of the continuum of care
- Improves efficiencies resulting in less waste and cost
- Positions the organizations for an unknown and evolving clinical and business environment
- Addresses fragmentation and poor transitions in care delivery
- Improves the ability to retain and recruit staff
- Develops loyal patients and families who spread positive word of mouth in the community
- Identifies solutions that drive down costs in a way that protects and improves outcomes and experiences
PFCC in Action: Reducing Readmissions
A perfect example of the power of this approach can be seen at Magee-Womens Hospital of UPMC in the Bariatrics PFCC M/P Working Group. As one of its PFCC projects, this group analyzed reasons for readmissions within 30 days and noted a common thread of dehydration. Shadowing (real-time direct observation which is Step 3 of the PFCC M/P) identified appropriate time points and methods of improving hydration education, which led to the following PFCC projects:
- Development of a quiz to assess patient understanding regarding dehydration prior to discharge
- Development of a Hydration Fact Sheet (with input from patients and families.
- Staff education on the “teach-back” technique
- Development of a Bariatric Surgery Discharge Journal to log fluid intake (and to log wound assessment, pain score, nausea assessment, signs/symptoms of dehydration, and fluid/ml ounce conversation tables)
- Distribution of “calibrated” water bottles.
- Nursing post-operative calls and assessment of journals
This PFCC Working group also increased their focus on the other common complications that result in readmission within 30 days after bariatric surgery — wound infection, pain, vitamin deficiency, weight gain and deep vein thrombosis. The improved patient education program increased collaboration between inpatient and outpatient clinical teams and disciplines as well as collaboration with other Bariatrics programs in the same health system.
A Win-Win
Post-implementation results were significant. Readmissions within 30 days were reduced from an average of 9.5 per month to 1 per month in the initial 22 patient intervention group; these results have been sustained. Decreasing readmissions has ramifications for decreased infections and other clinical outcomes that further reduce the cost of care as well. It’s been a win-win. The hospital has been able to avoid the financial hit for unnecessary readmissions and the patients and families are able to return to pre-surgical levels of activity and work sooner.
There are many examples of how the PFCC M/P improves outcomes and experiences and lowers costs. It’s been successfully implemented in areas as diverse as trauma, outpatient mental health services, oncology, home health care, total joint replacement and more. So it turns out that doing the right thing aligns perfectly with the business case for patient- and family-centered care.
Editor’s note: For an overview of the six-step PFCC Methodology and Practice, download our infographic. For more detailed information, contact Pam Greenhouse at greenhousepk@upmc.edu or visit the PFCC website.





1 Comment
Thanks for your incite!
1 Trackback