
Unintentional overdose deaths due to prescription narcotics have quadrupled since 1999 and now outnumber those involving heroin and cocaine.[i],[ii] As a result, such misuse of medications has been accurately described as a national epidemic by the CDC and consumes over $70 billion in health care costs. [iii],[iv]
Controlling patients who frequent the emergency department (ED) for unnecessary narcotic prescriptions is a critical form of patient engagement. Though challenging, it can be accomplished through process change and technology.
Identifying ‘Frequent Flyers’
 ED frequenters — those with four or more visits within the most recent year– comprise 6 % of ED patients and 25% of ED visits.[v] The largest cohort is narcotic seekers, that is, those patients trying to obtain opioid pain relievers for nonmedical use or abuse. They often lack access to a primary care provider and present themselves with an acute exacerbation of a painful condition. It is hard to know if the real issue is physical dependence, financial dependence (selling) or enabling another’s dependence, but practitioners can usually sense when a narcotic prescription is not what’s best for the patient. State prescription databases and registries of frequent ED visitors have made it much easier to establish a pattern of frequent narcotic dispensing.
ED frequenters — those with four or more visits within the most recent year– comprise 6 % of ED patients and 25% of ED visits.[v] The largest cohort is narcotic seekers, that is, those patients trying to obtain opioid pain relievers for nonmedical use or abuse. They often lack access to a primary care provider and present themselves with an acute exacerbation of a painful condition. It is hard to know if the real issue is physical dependence, financial dependence (selling) or enabling another’s dependence, but practitioners can usually sense when a narcotic prescription is not what’s best for the patient. State prescription databases and registries of frequent ED visitors have made it much easier to establish a pattern of frequent narcotic dispensing.
The Challenges of Engagement
Suggesting that dependence or addiction is the primary underlying problem, turns an otherwise quick and pleasant interaction into an emotional confrontation. However, doing so is the only way to disrupt the normative cycle. Because it is well established that ‘lock-in programs’ with access to one prescriber and one pharmacy are effective at reducing the overdose risk and unnecessary ED visits, then it can be inferred that shying away from confrontation and overprescribing is substandard medicine. [vi]
Facilitating Behavioral Change
Information systems can be leveraged to facilitate behavior change. EMRs can incorporate frequent visitor flags and patient-specific care plans. The flag should be evident to the care team as soon as the patient appears tracking system. This prompts review of the specific care plan.
It is important to make the patient aware that a visit flag and a care plan will be created. As a bridge, some will prescribe a modest number of narcotic tablets while making it clear that no further narcotics will prescribed thereafter (unless, of course, warranted by an entirely new situation). Establishing and enforcing such rules are paramount in changing behavior.
It is wise to inform senior administrators and medical staff leaders that efforts to restrict narcotic prescribing are commencing since a flurry of complaints is sure to follow. Ideally, the hospital CEO should publicly endorse the effort.
Checklist for Taking Control
To summarize the steps involved in controlling narcotic seekers, consider the mnemonic, NARC.
N – Notice the Pattern
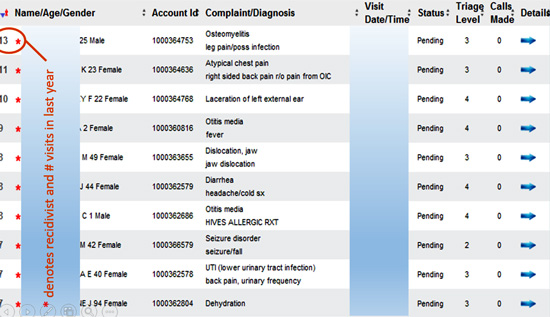
There are common threads with narcotic seekers. These include NSAID allergies, history of one or more painful conditions, exaggerated or feigned symptoms, frequent visits and lack of a picture ID. The most important factors is prescription history and ED use patterns. State prescription databases and frequent visitor registries are invaluable, as shown in the partial screen shot below which was taken from SMARTworks®-EffectiveResponse.
A – Address the Concern
Narcotic dependence is insidious, common and difficult to control. It is wise to speak with the primary care physician or specialist who knows the patient. Patients reliably become angry and defensive when the issue is exposed. Accompanying family members may be conflicted between advocating for their loved one and acknowledging their own suspicions. Being perceived as a mindful, empathetic caretaker is best when engaging narcotic seekers.
|
R – Refuse to Prescribe
Despite being uncomfortable in withholding something the patient can only get from a practitioner, do not give in. Use supportive data derived from national initiatives. C – Control Future Visits Use the EMR to flag the patient during future visits and house a specific care plan containing non-narcotic treatment strategies and follow-up options (see Sidebar example). Case managers are particularly helpful in assuring that care plans are developed and followed. They can also check on the patient’s well-being and follow-up compliance through post-visit phone calls or electronic messaging. |
|
References/Links
[i] National Institute on Drug Abuse Prescription Drugs: Abuse and Addiction. NIH Publication Number 11-4881. October 2011. http://www.drugabuse.gov/sites/default/files/rrprescription.pdf
[ii] High-Risk Use by Patients Prescribed Opioids for Pain and Its Role in Overdose Death. JAMA Intern Med. March 2014. http://archinte.jamanetwork.com/article.aspx?articleid=1840033
[iii] CDC Grand Rounds: Prescription Drug Overdoses — a U.S. Epidemic. MMWR 61(01) January 2012. http://www.cdc.gov/mmwr/preview/mmwrhtml/mm6101a3.htm
[iv] Prescription for Peril by the Coalition Against Insurance Fraud http://www.insurancefraud.org/prescription-for-peril.htm#.UzDD4_ldWa8
[vi] 2.3 Million Pills Off the Streets, $5.2 Million Saved by Narcotics Lock-in. North Carolina Department of Health and Human Services. May 2012 http://www.ncdhhs.gov/pressrel/2012/2012-05-14_pills_off_streets.htm






1 Comment
Its often hard to get proper tmnetraet for chronic illness, because a lot of time you look fine on the outside. Its like people forget there is a whole inside where havoc is going on.I grew up in Michigan and was diagnose with my first autoimmune disorder at the age of 15 (severe psoriatic arthritis). This was not surprising as my father had more that one AI problem including severe Chrons. The doctor I had in Michigan was fantastic. I had seen him basically my whole life. He took my pain very seriously and managed it well. Never made me feel like less of a person or untrustworthy. He never once humiliated me. I was his patient for over 20 years. I was also naive and though most other doctors treated their patients with this type of respect. Even the specialist referrals weren’t truamatic.I became disabled in 2005.I decided to move to California 3 years ago and boy did I find out things were different. I figured it would be easy just to transfer records and set up shop with a new doctor, I couldnt have been more wrong. I interviewed a lot of doctors upon arriving because I kept being called a liar, a drug seeker, that I didnt want to get better. I have MRI’s covering 8 years I brought to all these appointments that clearly showed the progression of the arthritis, along with degenerative disc disorder. I was still shoved out of their offices in tears because I wasnt being believed. Granted they would give me a script for the bare minimum when it came to pain management but didnt want to stick with the tmnetraet plan that actually gave me a life. One pain doctor wanted to cut me open before he saw the MRI’s. There is nothing surgically to do. He made sure to humiliate me every time I went in, once even handing me a urine cup when I know it wasnt in the contract! After him I continued to try and find a fit for me. Doctors came and went and it always seemed to go the same here is your pain medication, now here is your humiliation. In this time I developed Chrons and hypothyroid which were overlooked, because I wasnt taken seriously.I have finally put together a group of professionals I trust, starting with my GP. He treats my pain seriously and wants me to be comfortable even if it means I am in his office a lot. He ALWAYS calls back.He is also not afraid to be aggressive with it, and it was like that from the first visit. My GI doc is fantastic as well. I feel very safe now with my team. I also always take someone in the office with me because if I am going to be mistreated I want witnesses and someone who will speak up for me as I just tend to cry.Some of this medical hell has added to my PTSD, I was labeled a drug seeker, they treated me no better than my verbally abusive mother. Major illnesses were overlooked because of their bias. People shouldnt have to suffer because doctors have bias.Its not only doctors that have treated me this way. Nurses, pharmacists, etc. One pharmacist was so out of line my advocate reported him to the state board.If you are frustrated with your doc keep looking. I drive an extra 20 miles to see mine,I know not everyone can do that, it can be worth it though. It takes so much energy to be chronically ill that energy doesnt need to be wasted on medical professionals that dont want to help.